Treatment for Retinal Detachment in Baltimore
Also serving Pikesville, Catonsville, Glen Burnie, & Rosedale
 Treating retina detachment is one of our special areas of service here at Elman Retina Group. When a retina becomes detached, surgery is necessary to replace it in its proper position. It takes highly trained specialists like us to do this properly. Your eyes are precious, so don’t trust their repair and healing to anyone but the best. Come to us for a consultation and let us show you just what we can do and how well we will care for your eyes.
Treating retina detachment is one of our special areas of service here at Elman Retina Group. When a retina becomes detached, surgery is necessary to replace it in its proper position. It takes highly trained specialists like us to do this properly. Your eyes are precious, so don’t trust their repair and healing to anyone but the best. Come to us for a consultation and let us show you just what we can do and how well we will care for your eyes.
What is Retina Detachment and What Does it Do to Your Vision?
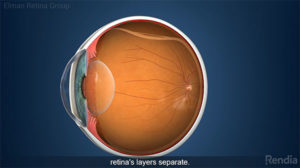
The retina is in the back of your eye, and is composed of light-sensitive tissue. If it is detached, this means it is not properly attached to the surrounding tissues anymore. It may also mean the retina has a tear or a hole in it. Sometimes, a tear or hole in the retina forms first, and causes the retina to detach from the surrounding tissues if it is not treated. In any of these instances, the damage to the retina must be repaired.
In fact, it must be repaired quickly. Detached retina tissue quickly becomes useless due to cells in it dying off. When enough retina cells are gone, it can lead to blindness in the affected eye. A tear or hole in the retina can be repaired with a laser, if the damage appears before the retina itself detaches. If the retina begins to detache, more complex surgery, called a pneumatic retinopexy, must be done to repair and correct it.
With this type of surgery, a gas bubble is injected into the eye, and the bubble floats to the retina and pushes it back into its proper place. A laser will be used to seal it there, so it does not detach again.
 If the retina is severely detached, another type of surgery is used to correct it. Unlike the retinopexy, which is done in your eye doctor’s office, these other surgeries are done in a hospital or day surgery center.
If the retina is severely detached, another type of surgery is used to correct it. Unlike the retinopexy, which is done in your eye doctor’s office, these other surgeries are done in a hospital or day surgery center.
There are two other types of surgery used in a hospital or surgery center setting. One is the scleral buckle. With this method, the walls of the eye are pushed inward to meet the damaged part of the retina, sealing off the damage, and creating a smooth retina again. The second type of surgery is called a vitrectomy. This surgery inserts small devices into the eye to release the pressure on the retina. With the release of pressure, the retina can move back into its correct position on its own. Both surgical procedures are usually done with local anesthesia while you are awake, but can be done with general anesthesia if you prefer and if your eye doctor determines it is correct for you.
While the surgery needs to be done quickly to avoid any loss of vision, and the recovery can take several days to several weeks, depending on the type of surgery, the prognosis for retinal detachment surgery is typically very good for most patients. Eye health and overall health history play a part, but most patients do very well and have no complications.
Frequently Asked Questions about Retinal Detachment
What causes retinal detachment?
The retina can separate from the back of the eye due to different causes, resulting in severe vision loss.
The most common cause of retinal detachment is a tear or break in the retina. The vitreous, or gel-like fluid in the center of the eye, can then seep under the retina and push it away from the back wall of the eye. When the retina is detached from the inner eye wall, it cannot function properly, so vision is severely impaired.
Retinal detachment can also occur due to complications of diabetes. High blood sugar from diabetes can damage the blood vessels in the back of the eye, causing scarring. The scarring can pull on the retina, causing it to separate from the back of the eye.
Another cause of retinal detachment is a traumatic blow to the eye or another type of eye injury.
What are the symptoms of retinal detachment?
Symptoms of retinal detachment can include the following:
- A sudden increase in the number and size of floaters – i.e., tiny spots, specks or other objects that appear to float in the field of vision
- Flashes of light
- A “curtain” of darkness that moves over the field of vision
- Blurry vision
- Impaired peripheral (side) vision
Am I at risk of retinal detachment?
Although retinal detachment can happen to anyone, certain people are at higher risk. Risk factors include the following:
- A family history of retinal detachment or other retinal problems
- Serious eye injury
- History of complex eye surgery (e.g., complicated cataract surgery)
- Diabetes and diabetic retinopathy
- Near-sightedness
Can retinal detachment cause permanent vision loss?
Yes. If retinal detachment is not treated quickly, it can cause permanent vision loss and blindness.
Is there any way to lower the risk of retinal detachment?
The best thing you can do is have regular eye exams and be aware of the symptoms of retinal detachment. If you experience any symptoms, contact the eye doctors at Elman Retina Group as soon as possible. The earlier you seek medical care, the better your chances of avoiding permanent vision loss to retinal detachment.
Also, it is always wise to protect your eyes from a traumatic blow or injury by wearing safety goggles or protective eyewear while playing sports or engaging in other risky activities (e.g., doing yardwork or tasks around the house that involve projectiles).
How does an eye doctor diagnose retinal detachment?
Retinal detachment is diagnosed through a comprehensive dilated eye exam with our doctors at Elman Retina Group. After widening your pupil with special dilating eye drops, our doctors look inside your eye using a light magnification instrument. Magnification lenses, or a microscope called a slit lamp, may be used to get a better look. In some cases, an ultrasound or optical coherence tomography (OCT) eye scan may be taken to look at the retina.
What is the best treatment for retinal detachment?
The right treatment solution for retinal detachment depends on factors such as how much of the retina has detached, and which part is detached. Retinal tears or holes that have not yet caused the retina to detach can be treated with an in-office laser procedure. If the retina has detached, treatment options include an in-office pneumatic retinopexy, scleral buckle surgery and/or vitrectomy surgery. The treatment options often require injecting a gas bubble in the eye that remains in place up to a couple months. This helps the retina stay flat on the surface of the eye as it slowly heals.
What are the early warning signs of a detached retina?
The earliest warning signs often include a sudden increase in floaters, flashes of light in one eye, or a shadow appearing in your peripheral vision. Some patients describe it as a gray curtain slowly moving across their field of vision. These symptoms may begin before full detachment occurs and should always be treated as an emergency.
How quickly should retinal detachment be treated?
Retinal detachment requires urgent medical attention. The longer the retina remains detached, the greater the risk of permanent vision loss due to damage to light-sensitive cells. In many cases, surgery is scheduled as soon as possible — sometimes the same day or within 24 hours — depending on the severity and location of the detachment.
What causes floaters and flashes before a detachment?
Floaters and flashes are often caused by changes in the vitreous gel inside the eye. As the vitreous shrinks with age, it can tug on the retina. This traction may produce flashes of light or release small clumps of gel that appear as floaters. If traction creates a tear, fluid can pass beneath the retina, leading to detachment.
What is the difference between a retinal tear, hole, and detachment?
A retinal tear or hole is a break in the retinal tissue. When fluid passes through that break and separates the retina from the back of the eye, it becomes a retinal detachment. Treating a tear or hole early with laser photocoagulation or cryotherapy can often prevent a full detachment from developing.
When is vitrectomy chosen instead of scleral buckle?
The choice of procedure depends on the size, location, and complexity of the detachment. Vitrectomy is often recommended when there is significant vitreous traction or bleeding inside the eye. Scleral buckle surgery may be more appropriate for certain peripheral tears. In some cases, surgeons combine techniques to achieve the best outcome.
Can vision return fully after retinal detachment surgery?
Visual recovery varies. If the macula (the central part of the retina) remains attached at the time of surgery, the chances of preserving excellent vision are higher. If the macula were detached, some visual loss may persist even after successful repair. Improvement often continues gradually over several months.
What is the visual recovery timeline after surgery?
Vision may be blurry immediately after surgery, especially if a gas bubble is used. As the bubble slowly absorbs over several weeks, vision gradually improves. Full recovery may take several months, depending on the extent of the detachment and the type of procedure performed.
What should I avoid after retinal detachment surgery?
You may be instructed to maintain specific head positioning to keep a gas bubble in place. You should also avoid flying or visiting high-altitude locations until the gas bubble fully dissolves. Moreover, limit strenuous activity, heavy lifting, and bending during early recovery to prevent increased eye pressure.
Can retinal detachment happen again after treatment?
While surgery has a high success rate, recurrent detachment can occur in some patients. Close follow-up appointments allow retina specialists to monitor healing and detect new tears early if they develop.



